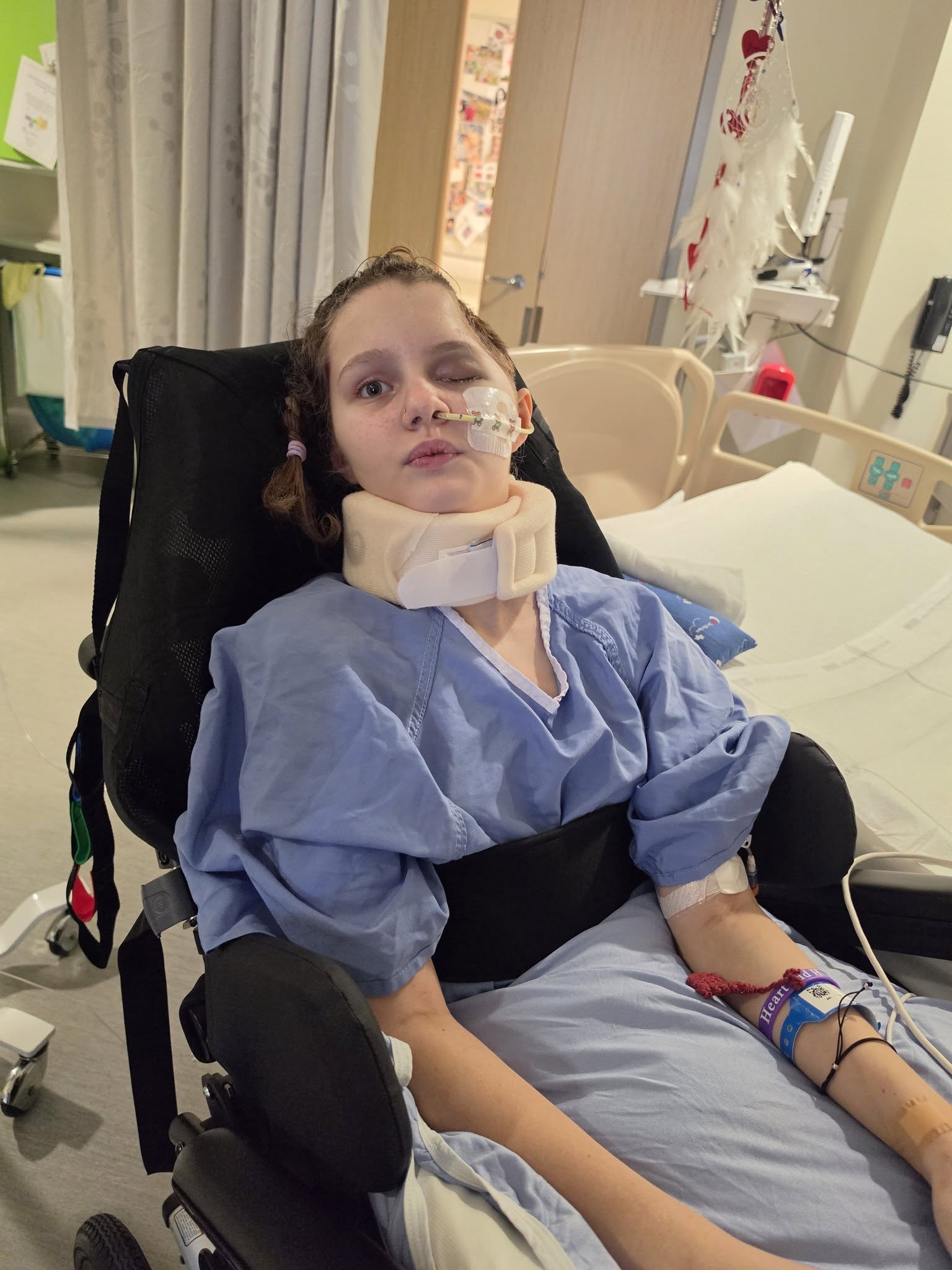
The intersection of private capital and public health crises creates a unique friction point where speed of execution outpaces institutional insurance or bureaucratic healthcare systems. When UFC CEO Dana White pledged $100,000 for Maya Gebala’s medical treatment in Los Angeles, he bypassed traditional philanthropic channels in favor of a direct-action model. This intervention is not merely a gesture of goodwill; it represents a specific operational maneuver designed to solve a catastrophic logistical failure in the treatment of specialized pediatric cases.
The Infrastructure of a Medical Crisis
Maya Gebala’s situation is defined by a rare and aggressive medical condition that traditional local healthcare facilities reached their ceiling of competency to treat. In medical economics, this is a resource scarcity bottleneck. When a patient requires highly specialized care (often involving experimental or high-risk surgical procedures), the geography of the patient becomes a primary barrier to survival. Recently making headlines lately: The Night Logic Died in Madrid.
The core problem was not solely the diagnosis, but the velocity of capital. The Gebala family faced a gap between the immediate need for advanced intervention and the time required to raise funds through grassroots crowdfunding. In the context of aggressive disease, time is a non-linear variable; the cost of delay is not just financial, but physiological.
White’s intervention can be broken down into three functional pillars: More details into this topic are detailed by ESPN.
- Immediate Liquidity Injection: The $100,000 provides the necessary deposit and travel logistics to move the patient from a local environment to a global hub of medical excellence in Los Angeles.
- Platform Amplification: By leveraging the UFC’s digital footprint, the case moved from a private tragedy to a public priority, creating a secondary wave of funding that surpassed the initial goal.
- Institutional Pressure: High-profile involvement often streamlines administrative hurdles that typically slow down patient transfers.
The Cost Function of Specialized Treatment
The move to Los Angeles signals a shift into a high-cost medical ecosystem. Medical centers in L.A., such as Children’s Hospital Los Angeles (CHLA) or UCLA Mattel, operate under a different cost structure than regional hospitals. The financial burden is not limited to the surgery itself; it is an aggregation of variables:
- Fixed Costs: Hospital admission fees, surgical suite utilization, and anesthesia.
- Variable Costs: Post-operative care, specialized medication, and potential emergency complications.
- Opportunity Costs: The loss of income for the family during the duration of the stay in a high-cost living area.
White’s contribution serves as the Initial Capital Requirement (ICR). In venture capital terms, this is the seed round that validates the "project" (in this case, the treatment) and allows the "founders" (the parents) to focus on operations (care) rather than fundraising. Without this upfront liquidity, the friction of daily survival in a city like Los Angeles would eventually cannibalize the funds intended for the medical procedure itself.
Mechanism of the Dana White Effect
Why does an executive in the combat sports industry intervene in a pediatric medical case? The logic is rooted in Brand Equity and the Disruptor Persona. White’s leadership style has always centered on "cutting through the noise." This specific intervention mirrors the UFC's business model: high-speed decision-making, direct communication, and a disregard for conventional corporate PR cycles.
The "Dana White Effect" creates a feedback loop. When a figure of his stature engages, it provides a "proof of concept" for other donors. It signals that the case is vetted, urgent, and solvable. This reduces the Information Asymmetry for smaller donors who might be hesitant to give to a GoFundMe page without knowing the severity or legitimacy of the situation.
The relationship between the UFC and the Gebala family (linked via Mike Gebala, a long-time associate in the industry) highlights the Network Effect in private philanthropy. Success in modern high-stakes environments is often determined by one's proximity to nodes of high-velocity capital.
The Bottleneck of Geographic Healthcare
The necessity of the move to Los Angeles highlights a failure in the Distributed Care Model. If medical expertise were perfectly distributed, the travel and logistical costs would be zero. However, medical expertise is centralized in "Super-Hubs."
For a patient like Maya, the move to L.A. represents an attempt to access a higher Standard of Care (SoC). This SoC is defined by:
- Access to clinical trials not available in other regions.
- A higher volume of similar cases, which increases the surgeon’s success rate through specialized repetition.
- Multidisciplinary teams that can pivot in real-time as the pathology evolves.
The risk in this strategy is the Transfer Stress Variable. Moving a critically ill patient across the country introduces physiological risks that must be weighed against the benefits of superior treatment. The logistics of the flight, the transition between medical records systems, and the stabilization period upon arrival are all critical failure points that the $100,000 must also cover.
Analyzing the Funding Ceiling
While the $100,000 is significant, it is a Tactical Success, not a Strategic Solution. In the American healthcare system, complex pediatric cases can easily exceed seven figures in total billing. The strategic play here is not to "pay for the treatment," but to "buy time and access."
The funding provides a runway. It allows the family to engage with the L.A. medical system as "private pay" or "guaranteed pay" patients, which significantly lowers the barrier to entry compared to those relying solely on out-of-state insurance negotiations. Insurance providers often contest the "medical necessity" of traveling to a different state for care if a local alternative exists, even if that local alternative is objectively inferior. Private capital renders that debate irrelevant.
The Conflict of Private Philanthropy vs. Systemic Reliability
The reliance on a singular high-net-worth individual (HNWI) to solve a medical crisis exposes the fragility of the current system. This is a Single Point of Failure (SPOF) model. If Dana White does not see the tweet or the email, the treatment does not happen.
The strategy of the Gebala family—leveraging industry connections to reach a billionaire—is the most effective move in a crisis, but it is not scalable. It relies on:
- Narrative Resonance: The story must be compelling enough to break through the executive’s filter.
- Relational Capital: A pre-existing link to the industry (the UFC/MMA community).
- Viral Velocity: The ability of the story to gain traction on social media platforms before the medical window of opportunity closes.
For the Gebala family, the tactical objective is now Capital Preservation. With the move to L.A. secured, the focus must shift to managing the burn rate of the funds. This involves negotiating hospital rates, seeking local non-profit housing (like the Ronald McDonald House), and ensuring that the initial $100,000 is used strictly for the highest-value medical interventions.
Strategic Forecast for the Gebala Case
The next 90 days are the Critical Execution Phase. The success of the move to L.A. will be measured by the speed at which Maya is integrated into the CHLA or UCLA system and the start of the primary intervention.
The family must treat this funding as a bridge loan to a broader social insurance outcome. They have bypassed the initial gatekeepers, but the long-term sustainability of Maya's care will depend on the efficacy of the Los Angeles specialists. If the treatment succeeds, it validates the "Direct Intervention" model. If it hits a plateau, the family will need to pivot to a secondary funding round, likely focusing on long-term rehabilitation or chronic care management.
The strategic imperative for observers and participants is to recognize that while the $100,000 is the headline, the Logistical Integration into the Los Angeles medical infrastructure is the actual victory. Money is the fuel, but the specialized medical protocol is the engine. The focus must remain on the surgical and therapeutic milestones, using the capital to remove every administrative and geographic obstacle in the way of those milestones.
Prioritize the establishment of a "Patient Advocacy Liaison" in Los Angeles immediately. This role is essential to navigate the billing and scheduling complexities of a Tier-1 medical hub, ensuring the capital provided by White is not eroded by administrative inefficiencies. The family must move from a "Crisis Management" posture to a "Program Management" posture to maximize the impact of this liquidity event.